
Foundational Principles of Modern Diabetes Management
The evolution of diabetes care is marked by a significant shift in clinical philosophy. For years, the American Diabetes Association's Standards of Care have progressively moved beyond merely treating hyperglycemia to embracing a proactive, technology-enabled, and patient-centered model. This fundamental change in perspective is not just academic; it directly dictates the selection and application of modern diabetes care supplies for professionals. The goal is no longer to react to isolated glucose readings but to build a comprehensive, predictive, and personalized management strategy for each patient.
At the heart of this new paradigm is the concept of an integrated data ecosystem. Today’s devices are not standalone tools. Instead, they communicate with one another, creating a continuous feedback loop that informs personalized treatment plans. A continuous glucose monitor, a smart insulin pen, and a patient’s smartphone app can work in concert to provide a detailed picture of glycemic patterns, something a simple logbook could never achieve. This interconnectedness transforms raw data into clinically actionable intelligence, allowing for more precise therapeutic adjustments.
This technological integration places new demands on the interdisciplinary care team. Physicians, specialist nurses, and dietitians must collaborate more closely than ever. Each professional’s expertise is crucial for selecting the right tools, training patients on their use, and interpreting the complex data they generate. We have seen firsthand that building such a skilled and cohesive team is fundamental to delivering modern diabetes care. It is why organizations must connect with top-tier talent, a mission we detail in explaining who we are and our commitment to quality healthcare staffing.
Of course, implementing this vision presents operational challenges for healthcare facilities. There is a constant need to balance the clinical benefits of advanced technology with budgetary constraints. Navigating the complexities of US reimbursement policies for devices like CGMs and insulin pumps requires dedicated administrative effort. Furthermore, clinics must maintain a diverse inventory of supplies to accommodate varied patient needs, preferences, and insurance formularies. Understanding these strategic realities is the first step in equipping a clinical practice for excellence in diabetes management.
Advanced Glucose Monitoring Technologies in Clinical Practice
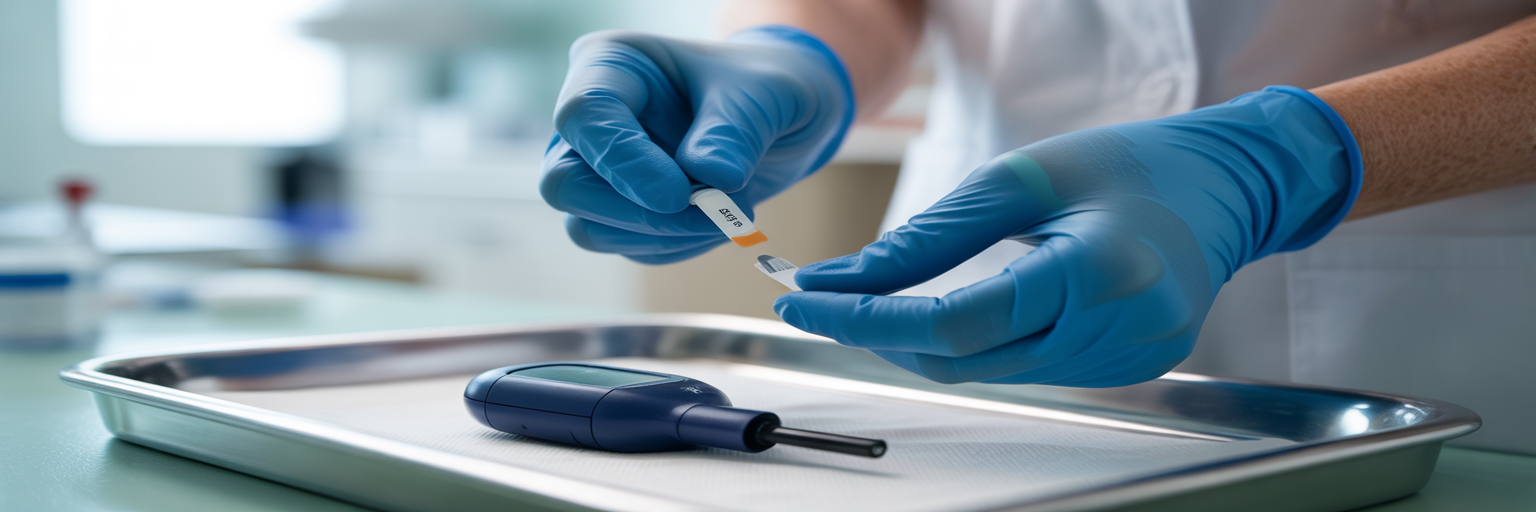
Building on the principle of data-driven care, the choice of glucose monitoring technology is one of the most critical decisions in a patient's treatment plan. The conversation has moved far beyond simply checking blood sugar. It now centers on the quality, depth, and continuity of the data obtained. The distinction between traditional Blood Glucose Meters (BGM) and advanced glucose monitoring tools like Continuous Glucose Monitors (CGM) represents a difference in diagnostic philosophy.
Clinical Comparison: CGM vs. BGM
A BGM provides a single, point-in-time snapshot of capillary glucose. It answers the question, "What is the glucose level right now?" This is essential for immediate decisions, such as confirming a suspected low or calculating a pre-meal insulin dose. In contrast, a CGM provides a continuous stream of data, revealing trends, patterns, and the rate of glucose change. It answers the question, "Where is the glucose heading and how fast?" This dynamic view is diagnostically superior for identifying nocturnal hypoglycemia, postprandial spikes, and overall glycemic variability, insights that are often missed with intermittent fingersticks.
| Attribute | Traditional Blood Glucose Meter (BGM) | Continuous Glucose Monitor (CGM) |
|---|---|---|
| Data Type | Point-in-time capillary glucose reading | Continuous interstitial fluid glucose data (every 1-5 mins) |
| Clinical Insight | Provides a single snapshot; useful for immediate decisions (e.g., pre-meal) | Reveals trends, patterns, and glycemic variability over 24 hours |
| Key Metric | Single mg/dL value | Time in Range (TIR), Glycemic Variability (GV), trend arrows |
| Ideal Use Case | Cost-sensitive patients, those on oral agents, or as a CGM backup | Type 1 diabetes, complex insulin regimens, hypoglycemia unawareness, gestational diabetes |
| Patient Burden | Requires frequent, deliberate fingersticks | Requires sensor insertion every 7-14 days; may require calibration |
| Hypoglycemia Detection | Reactive; only detects if a test is performed during an event | Proactive; predictive alerts can warn of impending lows |
This table outlines the fundamental differences in data output and clinical application between BGM and CGM systems, guiding professionals in selecting the appropriate technology based on patient-specific needs and therapeutic goals.
Interpreting Advanced CGM Metrics
Effective use of CGM technology requires moving beyond just the glucose number. Professionals must master key metrics that offer a more holistic view of glycemic control. Time in Range (TIR), the percentage of time a patient spends within their target glucose range, has become a primary endpoint in clinical practice. It complements HbA1c by providing a day-to-day measure of stability. Equally important are Time Below Range (TBR), which quantifies hypoglycemic exposure, and measures of Glycemic Variability (GV), which reflect the amplitude of glucose swings. Analyzing these metrics allows for targeted adjustments to insulin regimens, diet, and lifestyle that a single HbA1c value cannot inform.
Patient Selection Criteria and Technical Management
While CGM offers significant benefits, it is not universally appropriate. Ideal candidates often include:
- Individuals with Type 1 diabetes.
- Patients on intensive insulin therapy, regardless of diabetes type.
- Those with a history of severe hypoglycemia or hypoglycemia unawareness.
- Pregnant individuals with diabetes.
Innovations and Standards in Insulin Delivery Systems
As glucose monitoring has become more sophisticated, so too have the methods for administering insulin. The landscape of insulin delivery devices 2026 and beyond is characterized by smart technology designed to reduce user error and improve glycemic outcomes. These innovations offer greater precision and data integration, but they also require a higher level of clinical expertise to manage effectively.
The Rise of Smart Insulin Pens
Smart insulin pens represent a significant step forward from their traditional counterparts. While they deliver insulin via a familiar pen format, their key innovation is data tracking. These devices automatically record the time and amount of each dose, transmitting this information to a smartphone app. This simple function helps prevent two of the most common and dangerous patient errors: dose stacking (taking doses too close together) and missed doses. For clinicians, the logged data provides an accurate record of insulin administration, making it far easier to identify reasons for glycemic excursions.
Tethered Pumps vs. Patch Pumps
For patients requiring continuous subcutaneous insulin infusion, the choice often comes down to a tethered pump or a patch pump. Tethered pumps consist of a main device connected to an infusion site on the body via thin tubing. They typically have a larger insulin reservoir and offer direct on-device controls. Patch pumps, conversely, are worn directly on the skin and contain both the insulin reservoir and infusion mechanism in a single, disposable unit controlled by a separate wireless device. The decision involves clinical and lifestyle trade-offs. A patient's activity level, comfort with visible tubing, and preference for on-body technology all play a role in this highly personalized choice.
Automated Insulin Delivery (AID) Systems
The most advanced systems available are Automated Insulin Delivery (AID), or "hybrid closed-loop," systems. These devices integrate a CGM and an insulin pump with a sophisticated control algorithm. The algorithm uses real-time CGM data to automatically adjust and deliver basal insulin, helping to mitigate highs and prevent lows with minimal user intervention. Clinical evidence consistently shows that AID systems significantly improve Time in Range and reduce the burden of daily diabetes management. They represent a major milestone in replicating the function of a healthy pancreas.
The Enduring Role of Traditional Methods
Despite these technological advancements, it is a clinical mistake to dismiss traditional syringes and vials. These methods remain critically important. They serve as an essential backup for every pump user in case of device failure or infusion site issues. For some patients, cost, insurance coverage, or technology complexity make pumps and smart pens inaccessible. Proficiency in teaching and managing insulin therapy with a syringe is not an outdated skill; it is a fundamental component of comprehensive diabetes care. The advanced skills needed to manage this full spectrum of delivery systems are highly valued, making this expertise a key differentiator for professionals seeking specialized healthcare jobs.
Point-of-Care and Complication Screening Tools
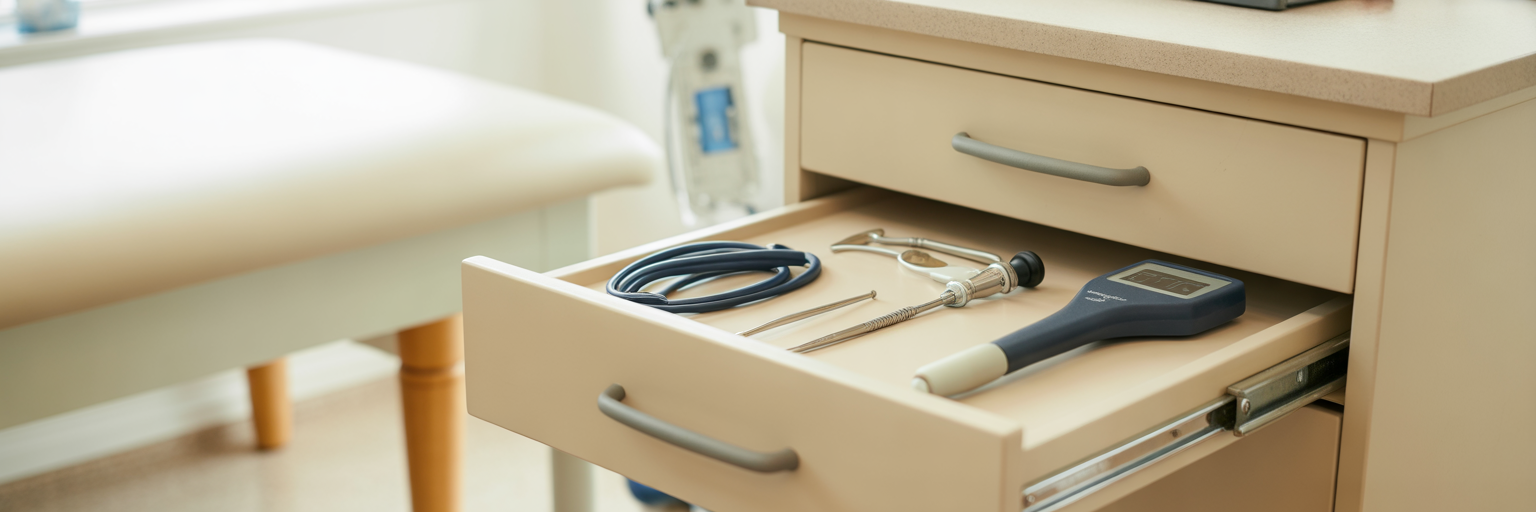
A complete set of diabetes care supplies for professionals extends beyond daily glucose and insulin management. It must include tools for the early detection and prevention of acute and chronic complications. Integrating point-of-care testing and standardized screening protocols into routine visits is essential for preserving long-term patient health and represents a core function of proactive care.
A prime example is ketone testing. While urine strips have been used for decades, they only measure acetoacetate and can lag behind the actual metabolic state. Blood ketone meters, which measure beta-hydroxybutyrate, provide a real-time, quantitative assessment of ketosis. This superior accuracy is critical for the early detection of diabetic ketoacidosis (DKA), allowing for timely intervention before a patient requires emergency care. Similarly, point-of-care HbA1c analyzers enable clinicians to have immediate, data-informed conversations with patients about their glycemic control over the past three months, facilitating on-the-spot adjustments to the care plan.
For annual complication screenings, a set of simple, low-tech tools remains indispensable. Every clinic managing patients with diabetes should have:
- A 10-gram monofilament to assess for loss of protective sensation, a key indicator of diabetic peripheral neuropathy.
- A 128-Hz tuning fork to test vibration sense, which is often one of the first sensory modalities to be lost in neuropathy.
Vascular assessment is another critical component. Handheld Doppler ultrasound devices are invaluable for screening for Peripheral Artery Disease (PAD) by calculating the Ankle-Brachial Index (ABI). This assessment provides a clear indication of lower extremity perfusion. Of course, a comprehensive physical exam also relies on fundamental diagnostic skills, and a quality stethoscope for auscultation of cardiac and vascular sounds is a staple of any complete clinical evaluation. Finally, proactive foot care involves prescribing appropriate supplies, such as non-occlusive moisturizers to maintain skin integrity and, for patients with venous insufficiency or edema, properly fitted medical compression socks to support vascular health.
Essential Patient Education and Self-Management Resources
The most advanced supplies are ineffective if the patient cannot use them correctly. Therefore, a core responsibility of the healthcare professional is to serve as an educator, and this requires a dedicated set of diabetes patient education resources. These tools bridge the gap between clinical instruction and real-world application, empowering patients to manage their condition confidently.
Hands-on teaching aids are particularly effective. Using an anatomically correct insulin injection pad allows patients to practice the physical technique of an injection in a safe, controlled environment. Portion-control plates and realistic food models are invaluable for teaching carbohydrate counting, transforming abstract dietary advice into a tangible, visual guide. These tools help demystify complex concepts and build muscle memory for daily self-care tasks.
In addition to physical aids, professionals must guide patients through the digital health landscape. This involves curating a list of reputable diabetes management apps and teaching patients how to evaluate them based on criteria like ease of use, data security, and clinical accuracy. It is no longer enough to simply recommend "an app"; we must equip patients to be discerning digital consumers. A critical aspect of this is ensuring resources are appropriate for a diverse patient population. This means providing materials in multiple languages, such as Spanish, and in accessible formats like large print or simple, visual-heavy guides to accommodate varying levels of health literacy.
A crucial area of education is hypoglycemia management. Every patient on insulin or sulfonylureas must have a clear plan and the right supplies. A professional's teaching kit should include:
- Examples of fast-acting glucose, such as tablets, gels, or liquids, to treat a low.
- Demonstration units for modern glucagon administration options, including pre-filled syringes, auto-injectors, and nasal glucagon, which have greatly simplified emergency treatment.
- Training kits to ensure family members or caregivers are prepared and confident to act in an emergency.
Integrating Supplies into Comprehensive Care Plans

The ultimate goal is to synthesize these individual supplies and technologies into a cohesive, personalized care plan. This requires moving beyond a one-size-fits-all approach and using clinical diabetes management tools to create customized "toolkits" for different patient archetypes. For example, a newly diagnosed Type 2 patient might start with a BGM, oral medications, and educational resources on diet. In contrast, a tech-savvy Type 1 athlete will require an AID system, a plan for managing exercise, and emergency hypoglycemia supplies. An elderly patient with visual impairments may benefit most from a simple insulin pen with an audible click for dose counting and a talking glucose meter.
From an operational standpoint, clinics must practice diligent inventory management. This includes forecasting supply needs based on the patient population and setting par levels for critical items like CGM sensors and insulin pump infusion sets to prevent stockouts that could disrupt patient care. Ensuring the clinical team is also well-equipped is part of this operational readiness, which includes maintaining an adequate stock of professional essentials like high-quality scrubs for the clinical team.
Proper documentation is the glue that holds this process together. Recording the specific supplies provided and the patient training conducted within the Electronic Health Record (EHR) ensures continuity of care and provides the necessary documentation for billing and reimbursement. This detailed record is invaluable when another team member sees the patient or during care transitions.
Finally, the healthcare professional's role extends to addressing patient access and affordability. This is often the most challenging part of the job. It involves helping patients navigate complex insurance formularies, complete prior authorization paperwork, and connect with patient assistance programs. In this capacity, the clinician acts not just as a provider but as a dedicated patient advocate. This holistic approach, which combines clinical expertise with practical support, is the hallmark of exceptional diabetes care. Building teams capable of delivering this level of service is the focus of comprehensive healthcare staffing services that understand the multifaceted demands of modern medicine.
