
Foundational Technologies in Autoimmune Disease Management
According to the National Institutes of Health, autoimmune diseases affect more than 24 million people in the United States, a figure that underscores the significant clinical challenge these conditions represent. The management of these diseases has undergone a profound transformation, moving away from generalized treatments toward highly specific interventions. This evolution is not just a matter of pharmacology but is fundamentally enabled by the development of advanced medical equipment designed to navigate the complexities of the human immune system.
The Complexity of Autoimmune Pathophysiology
The term "autoimmune disease" is an umbrella for over 80 distinct conditions, from rheumatoid arthritis to multiple sclerosis and lupus. Each disease presents a unique pathophysiological profile, meaning a one-size-fits-all diagnostic and treatment approach is clinically ineffective. This heterogeneity demands tools that can provide detailed, condition-specific information, moving beyond simple symptom observation to molecular-level analysis. The clinical need is for technology that can differentiate between closely related conditions and identify the specific immune pathways driving a patient's illness.
Shifting from Symptom Management to Precision Medicine
Historically, autoimmune care relied on broad immunosuppressants that, while sometimes effective, carried significant risks of infection and other side effects. The current paradigm is precision medicine, which involves using targeted biologic therapies that act on specific components of the immune system. This shift is entirely dependent on data. Clinicians require precise biomarker information to select the right therapy for the right patient, monitor its effectiveness, and adjust treatment protocols. Modern medical equipment provides the engine for this data-driven approach, turning molecular insights into clinical action.
The Clinical Imperative for Specialized Equipment
Standard hospital equipment often lacks the sensitivity and specificity required for modern autoimmune management. For instance, detecting the subtle immune markers that signal early disease activity or predict a flare requires high-sensitivity assays that go beyond the capabilities of conventional lab instruments. Effective management requires sophisticated autoimmune disease diagnostic tools that can quantify low-concentration cytokines and identify specific autoantibodies with high precision. Similarly, the safe administration of potent biologic drugs necessitates delivery systems with advanced safety features, far exceeding the requirements for standard intravenous fluids.
Economic and Operational Considerations for Facilities
For healthcare administrators, acquiring specialized equipment may seem like a significant capital expense. However, it is more accurately viewed as a strategic investment. By enabling earlier and more accurate diagnoses, these technologies can reduce the long-term costs associated with managing disease complications and hospitalizations. Furthermore, a facility equipped with state-of-the-art technology enhances its reputation, attracting both patients and top-tier medical talent. Yet, technology alone is not a complete solution. Optimizing a clinic's capabilities involves pairing the right tools with the right people. Ensuring the facility is staffed with professionals who can leverage these advanced systems is critical, a challenge where specialized recruitment support, such as the option to hire a healthcare contract recruiter, becomes invaluable.
Advanced Diagnostic Instruments in Clinical Immunology
The cornerstone of modern autoimmune care is the ability to accurately diagnose, monitor, and stratify patients based on detailed immunological data. This requires a suite of advanced diagnostic instruments that provide insights at the cellular and molecular levels. These technologies have moved clinical immunology from a largely observational field to one defined by quantitative analysis and objective metrics, empowering clinicians to make more informed decisions.
High-Throughput Flow Cytometers
High-throughput flow cytometers are essential pieces of advanced immunology lab equipment for detailed immunophenotyping. These instruments can analyze millions of individual cells, identifying and quantifying specific lymphocyte subsets such as Th17 and regulatory T-cells (Tregs). This information is critical for diagnosing and monitoring conditions like systemic lupus erythematosus (SLE) and multiple sclerosis (MS), where the balance of these cell populations is disturbed. The multi-parameter data generated by flow cytometry provides a detailed snapshot of a patient's immune status, guiding therapeutic choices. The sophisticated operation of these platforms requires highly trained laboratory professionals, highlighting the continuous demand for specialized talent found in listings for healthcare jobs.
Next-Generation Digital ELISA and Ultrasensitive Immunoassays
Traditional immunoassays often lack the sensitivity to detect the low-concentration biomarkers characteristic of early or subclinical autoimmune disease. Next-generation platforms, such as Single Molecule Array (Simoa), overcome this limitation. These ultrasensitive immunoassays can achieve picogram-level sensitivity, enabling the detection of minute quantities of cytokines, neurofilaments, and autoantibodies. This capability allows for earlier diagnosis, more precise monitoring of disease activity, and the potential to predict treatment response before clinical symptoms change.
Point-of-Care (POC) Autoimmune Testing Devices
While centralized labs provide deep analytical insights, the need for rapid, actionable data in the outpatient setting is equally important. This is the role of point of care autoimmune testing devices. These compact, automated analyzers can measure key inflammatory markers like C-reactive protein (CRP) and fecal calprotectin within minutes from a small sample. For a rheumatologist managing a patient's treatment or a gastroenterologist assessing a Crohn's disease flare, this immediate feedback allows for on-the-spot adjustments to therapy, improving patient outcomes and clinic efficiency.
Genomic and Proteomic Analysis Platforms
The future of personalized medicine in autoimmunity lies in genomics and proteomics. These platforms analyze a patient's genetic predispositions and protein expression profiles to stratify them into distinct biological subgroups. While still primarily used in research and specialized clinical centers, this information is beginning to help predict which patients will respond to certain biologic therapies. Although the complexity of data interpretation remains a challenge, these technologies hold the promise of moving beyond treating a named disease to treating an individual's specific molecular pathology.
| Technology | Primary Clinical Application | Key Advantage | Operational Setting |
|---|---|---|---|
| High-Throughput Flow Cytometry | Detailed immunophenotyping of cell subsets (e.g., T-cells, B-cells) | Provides multi-parameter analysis of millions of individual cells | Centralized clinical laboratory |
| Ultrasensitive Immunoassays (e.g., Simoa) | Detecting low-concentration biomarkers (cytokines, neurofilaments) | Enables earlier diagnosis and subclinical disease monitoring | Centralized clinical laboratory |
| Point-of-Care (POC) Analyzers | Rapid measurement of inflammatory markers (e.g., CRP, Calprotectin) | Provides actionable data within minutes during a patient visit | Outpatient clinic, infusion center |
| Genomic/Proteomic Platforms | Identifying genetic predispositions and protein signatures for patient stratification | Supports personalized medicine and prediction of therapy response | Primarily research, transitioning to specialized clinical labs |
This table outlines the distinct roles and advantages of key diagnostic platforms in autoimmune care. The data highlights how each technology addresses a different clinical need, from deep cellular analysis in a lab to rapid decision-making in a clinic.
Precision in Biologic and Infusion Therapy Administration
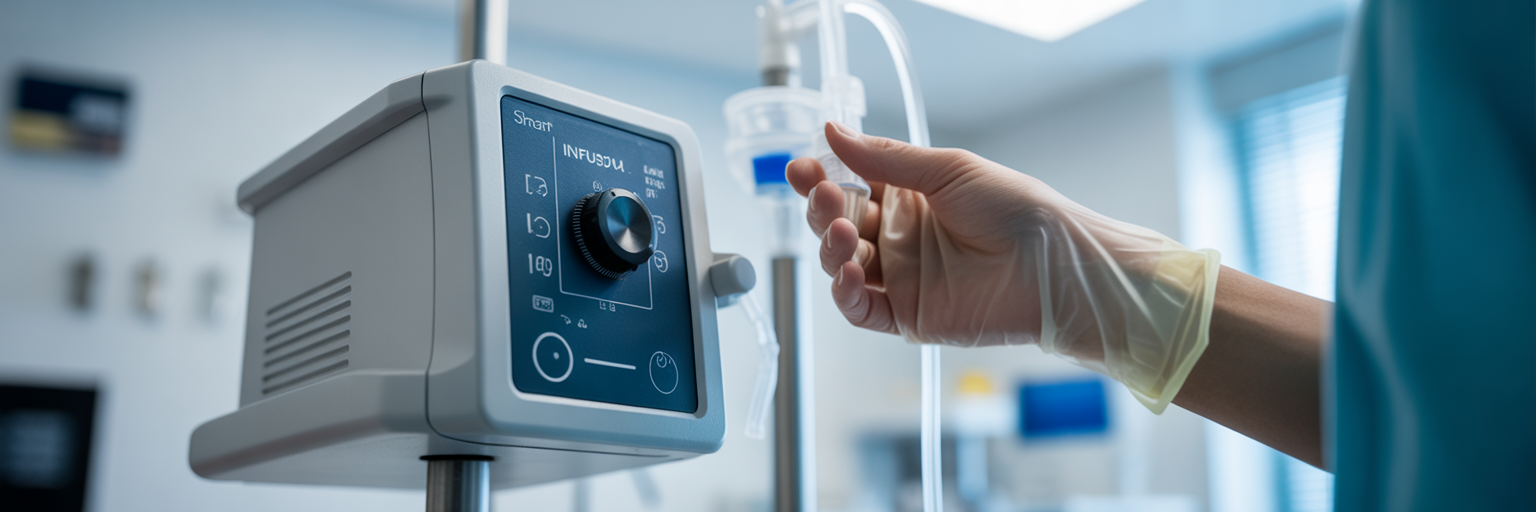
The therapeutic power of modern biologics is matched by their potential for adverse events if not administered correctly. Precision in delivery is not just a preference but a clinical necessity. The equipment used to administer these potent medications must incorporate advanced safety features to protect patients and ensure that the intended therapeutic effect is achieved without complication. This focus on safety and accuracy defines the modern infusion suite.
Smart Infusion Pumps with Dose Error Reduction Systems (DERS)
Smart infusion pumps are the standard of care for infusion therapy equipment for clinics administering biologics. Their most critical feature is the Dose Error Reduction System (DERS), which uses a customizable drug library to create safety guardrails for high-risk medications. Before an infusion begins, the pump verifies that the programmed parameters fall within pre-set limits. These safety checks include:
- Dose limits to prevent significant over or under-dosing.
- Rate controls that ensure the medication is infused over the correct duration.
- Concentration checks to confirm the drug is mixed correctly. This system acts as a crucial electronic second check, significantly reducing the risk of medication errors.
Wearable, Large-Volume Injectors for Subcutaneous Biologics
A significant development in treatment convenience and adherence is the rise of wearable, large-volume injectors. These biologic therapy administration devices allow for the subcutaneous delivery of medications that were previously only administrable via intravenous infusion. Patients can apply a small, on-body device that automatically delivers the dose over a set period, often in the comfort of their own home. This technology not only improves the patient's quality of life but also frees up valuable chair time in infusion centers, allowing facilities to focus resources on more complex cases.
Vascular Access and Visualization Technology
Patients with chronic autoimmune diseases often require frequent infusions, which can lead to difficult venous access over time. To address this, clinics increasingly use vascular access and visualization technology, such as ultrasound guidance for peripheral IV placement. An ultrasound probe allows the clinician to visualize the patient's veins in real time, guiding the needle to the target vessel with precision. This technique reduces the number of failed attempts, minimizes patient discomfort, and preserves venous integrity for future treatments.
Closed-System Transfer Devices (CSTDs) for Hazardous Drug Handling
Many immunomodulating drugs are classified as hazardous, posing a risk to the healthcare professionals who handle them. Closed-System Transfer Devices (CSTDs) are engineered to prevent exposure during drug preparation and administration. These devices create a sealed pathway from the drug vial to the patient, containing any aerosols or vapors that might otherwise escape. Using CSTDs is a key component of compliance with USP <800> standards for hazardous drug handling. This commitment to professional safety extends to personal protective equipment, where wearing appropriate clinical attire, such as a high-quality scrub, is fundamental to maintaining a safe and professional environment.
The Role of Continuous Patient Monitoring Systems
The management of chronic autoimmune disease extends far beyond the walls of the clinic. Technology now allows for continuous oversight and data collection, enabling care teams to monitor patients proactively and intervene before minor issues become major complications. These systems bridge the gap between appointments, providing a more complete picture of a patient's health status over time.
Remote Patient Monitoring (RPM) for Chronic Care Management
Remote patient monitoring systems are platforms designed to collect health data from patients in their daily lives. For autoimmune disease management, this can include patient-reported outcomes (PROs) about pain, fatigue, and function, as well as data from connected medical devices like blood pressure cuffs, smart scales, and pulse oximeters. This information is transmitted securely to the clinical team, providing regular updates on the patient's condition between scheduled visits and helping to identify trends that might otherwise go unnoticed.
Wearable Biosensors for Objective Data Collection
While consumer wearables track general activity, clinical-grade biosensors offer objective, medically relevant data. These are not the same as a fitness watch. For example, a small adhesive patch can continuously monitor skin temperature to detect a low-grade fever that might signal an impending disease flare. Similarly, motion sensors worn on a joint can quantify changes in range of motion and stiffness in a patient with rheumatoid arthritis, providing objective data to supplement subjective reports of pain. This granular information helps clinicians make more precise assessments of disease activity.
Integrated Telehealth Platforms for Virtual Check-ins
The data collected via RPM and biosensors becomes most powerful when integrated into a telehealth platform. This creates a system for proactive care. A typical workflow is as follows:
- Patient data from a wearable sensor or connected device automatically syncs to the platform.
- A pre-set algorithm flags a clinically significant deviation, such as a sustained increase in heart rate or a drop in oxygen saturation.
- The care team receives an automated alert through their clinical dashboard.
- A clinician can then initiate a secure video call to check in with the patient, assess the situation, and provide guidance.
Limitations and Data Overload Challenges
Despite their benefits, these systems present challenges. One of the most significant is the risk of data overload for clinicians. Without intelligent filtering and clear protocols, the sheer volume of incoming data can become overwhelming. It is essential for platforms to include algorithms that surface only the most clinically relevant information. Additionally, ensuring the security and privacy of patient data is paramount. All systems used in the United States must be fully compliant with HIPAA regulations, a key consideration for any facility implementing these technologies.
Integrating Equipment for Cohesive Clinical Workflows

Acquiring advanced medical equipment is only the first step. The true value of these technologies is realized when they are integrated into a cohesive ecosystem that supports efficient clinical workflows. A collection of standalone devices can create more problems than it solves, leading to data silos and administrative friction. The goal is to create a unified system where information flows seamlessly from the diagnostic lab to the infusion chair and the patient's home.
The Challenge of Interoperability
Interoperability, or the ability of different information systems and devices to communicate and exchange data, is the primary technical barrier to creating an integrated ecosystem. When a flow cytometer, an infusion pump, and a remote monitoring platform cannot speak the same digital language, clinicians are forced to reconcile data manually. This is inefficient and prone to error. Technical standards like Health Level Seven (HL7) and Fast Healthcare Interoperability Resources (FHIR) provide the foundation for solving this challenge, but implementation requires a strategic approach.
Centralized Data Dashboards and EMR Integration
The ideal state for a clinician is a single, centralized view of the patient. This means integrating data from all sources directly into the Electronic Medical Record (EMR). A well-designed dashboard within the EMR should allow a physician to see a patient's latest diagnostic results, review their infusion history, and track trends from their remote monitoring data on a single screen. This unified view supports holistic decision-making and eliminates the need to log in to multiple, disparate systems.
The Role of Middleware and Integration Engines
Middleware often serves as the "digital translator" that makes integration possible. These software layers sit between various medical devices and the EMR, converting data from proprietary formats into a standardized format that the EMR can understand. An integration engine can automate this process, ensuring that when a lab result is finalized or an infusion is completed, the relevant data is automatically filed in the correct patient's chart without manual entry.
Workflow Automation to Reduce Administrative Burden
An integrated system enables powerful workflow automation. For example, a critical lab result indicating a severe inflammatory response can be configured to automatically trigger an alert in the EMR and create a high-priority task for a nurse to schedule a telehealth follow-up. This reduces administrative burden and ensures that critical information is acted upon promptly. By automating routine tasks, these systems allow clinical staff to focus on high-value activities that require their expertise. A well-designed ecosystem supported by comprehensive staffing solutions ensures the right talent is in the right place, a core principle behind our services.
Future Horizons in Autoimmune Treatment Technology
The rapid pace of technological development continues to shape the future of autoimmune care. The tools and strategies of tomorrow will build upon the integrated systems being established today, moving toward a model of care that is increasingly predictive, automated, and personalized. While the technology evolves, the goal remains the same: to improve the lives of patients with chronic autoimmune conditions.
AI-Driven Predictive Analytics
As integrated data streams become more robust, the next frontier is using Artificial Intelligence (AI) to analyze this information. AI-driven algorithms will be able to identify subtle patterns in diagnostic, therapeutic, and patient-generated data to predict disease flares before clinical symptoms appear. This would enable preemptive interventions, such as a temporary medication adjustment or a targeted lifestyle recommendation, to prevent a full-blown flare-up and its associated complications.
Theranostics and Personalized Dosing
The concept of theranostics involves pairing a diagnostic test with a specific therapy to ensure optimal efficacy and safety. In the future, this could evolve into closed-loop systems for autoimmune care. Imagine a wearable sensor that continuously monitors the level of a biologic drug in a patient's bloodstream. This sensor could communicate with an implanted or wearable infusion device, which would then automatically adjust the dose in real time to maintain the drug within its optimal therapeutic window, personalizing dosing for each individual's unique metabolism.
Miniaturization and Non-Invasive Monitoring
Looking further ahead, technology will become less invasive and more seamlessly integrated into a patient's life. Researchers are developing microneedle patches that can painlessly sample interstitial fluid to analyze biomarkers without a traditional blood draw. Other innovations include optical sensors that may one day be able to measure inflammation through the skin. These advancements will make continuous monitoring easier and more comfortable for patients, providing an even richer stream of data for clinical management.
The future of autoimmune care is one where technology automates data collection, predicts clinical events, and personalizes treatment. Yet, even as these advanced systems become more prevalent, they will augment, not replace, clinical judgment. The foundational tools of clinical practice, from the physician's expertise to the simple but essential function of a high-quality stethoscope, will remain indispensable in the art and science of medicine.
